Somatic Experiencing is a specialized form of therapy that can help you resolve stress and trauma that may be contributing to health and relationship issues.
If you’re suffering from physical ailments, mental health issues or emotional struggles that are interfering with your relationships, your job and overall sense of well-being, unresolved trauma or a stress disorder could be to blame. The body’s nervous system often responds to chronic stress and trauma in a different way than the mind or thinking brain.
Consider this hypothetical situation:
Janet is a paramedic who deals with traumatic situations every day. As a first responder, she is trained to work under pressure, providing emergency care for people suffering from a range of wounds, illnesses and traumatic injuries to health crises like seizures, heart attacks and strokes —all while remaining calm and focused.
For years she feels she’s doing okay in her personal life. But, over time she begins to find herself in a distressing cycle of binge eating and a growing dependence on alcohol. Her relationship with her husband grows increasingly strained. She doesn’t sleep well. She begins to experience more body pain, like migraines, and her digestive system is a mess.
When asked if she’s experienced trauma, Janet replies “no” because in her mind (cortex or thinking brain), it’s her patients who have experienced trauma. However, Janet’s nervous system could be suggesting otherwise.
How does trauma impact health?
The common definition of trauma is defined as an emotional response to a terrible event like the loss of a child, war, abuse, sexual or physical assault, an accident or a natural disaster. Seventy percent of adults will experience at least one traumatic event in their lifetime (1).
BUT, this isn’t the only definition for trauma. It also refers to long-term dysregulation in the nervous system. This can happen due to many different factors including acute traumas and longer term experiences. Developmental trauma typically happens when there is recurrent abuse in childhood and chronic neglect or adversity in the home. Intergenerational trauma is another type of longer term trauma in which the oppressive or traumatic effects of an event are passed down to younger generations.
This long term dysregulation can occur even if the thinking brain is identifying experiences as “normal.” Even if you’re trained to respond to traumatic situations for your job—perhaps you’re in law enforcement, the military, firefighting, healthcare or part of a crisis response team— the body still needs a way to override the stress, terror and fear response to witnessing and/or having to manage a traumatizing experience.
Peter A. Levine, the author of Waking the Tiger, says that “trauma is not what happens to us, but what we hold inside in the absence of an empathetic witness”. In other words, it’s not the event itself but the physiological response to not having what we need in life experiences.
Unresolved trauma can increase a person’s risk for a variety of health issues, including anxiety, depression, PTSD, addictive behaviors, and physical ailments like digestive problems, cardiac issues, obesity, inflammatory diseases and cancer (2).
The pandemic further exacerbated trauma, including among healthcare workers faced with death every day, the families who never got to be with their loved ones when they died, and anyone who felt overwhelmed by the multitude of stressors brought on by COVID, from care taking to job security. In June 2020, The CDC reported that more than a quarter of adults 18 and older reported feelings of trauma and stress, and more than 40% were struggling with mental and behavioral health problems (3).
As mentioned, developmental trauma is the result of unresolved trauma that is rooted in childhood. As children, our first instinct in a threatening situation is to fight. If we can’t fight, the second thing we want to do is run away (flight). If we can’t do either of those things because the people in charge are bigger, stronger and an inescapable, regular part of our life, we freeze.
People with developmental trauma often learn to cope with stressful situations by freezing. They may not even realize they are doing it. For example, a child who was a victim of sexual abuse or an assault may struggle with intimacy as an adult even though they love and trust their partner. Their mind might be saying yes, but their body, recalling the trauma, is saying “absolutely not.”
How does chronic stress affect health?
In the chart below, you can see what happens when the body triggers the parasympathetic and sympathetic nervous systems to fight, flee, or freeze and the symptoms that are experienced in these different states.
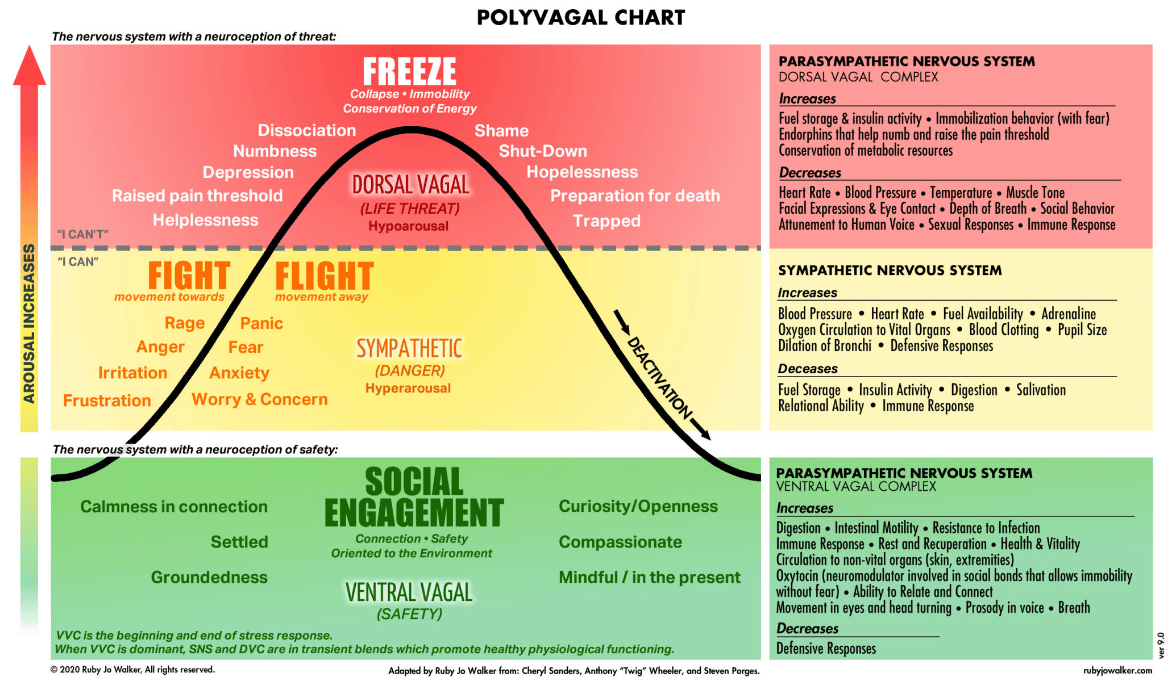
Our bodies and brains are hardwired for survival and don’t see a difference between modern-day stressors and the stress of being chased by a saber tooth tiger. So when we’re stuck in a stressful job, work for an abusive boss or feel trapped in a difficult relationship, we’re in a constant state of arousal —increased heart rate, high blood pressure, tunnel vision, tense muscles, slowed digestion, etc.
Because we often don’t complete the natural stress response, our bodies don’t resolve the fight, flight or freeze state. Our bodies then get stuck in the Sympathetic arousal and/or Dorsal Vagal dissociative state which sets us up for inflammation, digestive distress, and emotional and mental health struggles.
Somatic Experiencing therapists work to make the Ventral Vagal nervous system, which is the beginning and the end of the stress response cycle, dominant.
How is Somatic Experiencing different from talk therapy? Somatic Experiencing is a holistic approach developed by Dr. Peter Levine that helps people move through chronic stress and unresolved trauma by providing tools, resources and interventions that help the nervous system find safety again. It’s used by many different healing professionals to process and renegotiate trauma.
Somatic Experiencing teases apart the thinking brain (cortex) from the reptilian brain, which is where we store all of our felt experiences. It focuses on the bodily sensations that occur when our nervous system goes into fight, flight or freeze and helps the individual move back into a sense of safety.
Rather than just retelling (and often re-experiencing or feeling in the nervous system) a past trauma which is the traditional approach with talk therapy, Somatic Experiencing guides the client through a more embodied relationship to the event by bringing the sensations of the body into the conversation. This is done slowly and mindfully so that renegotiation can happen and progress to move through and beyond the experience can happen safely.
In the case of our paramedic, Janet, she may have been trained to deal with trauma calmly in the moment, but she didn’t have the coping skills for managing the traumatic energy that remains suppressed in her body after the event passes. And because the feelings associated with the traumatic events of her day-to-day job are uncomfortable, she numbs out with alcohol or seeks to feel pleasure again with food.
A Somatic Experiencing therapist would slowly help Janet identify the resources in her life that feel soothing and safe. Once this safety and calm is accessible, the therapist would then, over time, walk Janet through the bodily sensations that are aroused when she thinks about a traumatic event and help to renegotiate that event in the body. The result is that the lower brain and felt sense in the body feels that the event is over and resolved and safety has been found again. Through this process, Janet would also learn to recognize her body’s stress response and patterns in reaction and have strategies to move through them with greater ease. This ultimately builds resilience and the tools to avoid numbing the discomfort through substances like alcohol.
SIBAM. As a body-oriented approach, Somatic Experiencing relies on five elements referred to as SIBAM, an acronym that stands for:
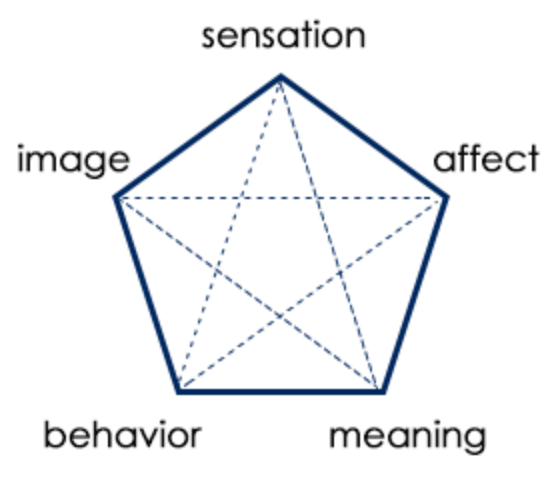
Sensation — your body’s response, like muscle tension, heart racing, stomachache, etc.
Image — the snapshots or pictures in the mind, the imagination
Behavior — observable non-verbal reactions, like gestures, facial expressions and posture.
Affect — emotions experienced in the body
Meaning — the words we use to make sense of an experience.
Somatic Experiencing can also help with stress disorders. According to the American Psychological Association’s 2020 Stress in America report, two out of three Americans report increased levels of stress. So even if you haven’t experienced a personally traumatic event, Somatic Experiencing can equip you with the tools you need to respond to and dial down stress (4).
For example, suppose you have a fear of public speaking.
- Your body might start to feel tense, your heart starts to race, and you start to sweat (Sensation).
- You can see the audience looking at you unsmiling and the room seems cold and dark (Image).
- Your knees start to quake and you cross your arms protectively (Behavior).
- You feel scared, and terrified, and strangely ashamed (Affect).
- You attach meaning to this fear by recalling an incident in childhood when a teacher publicly criticized you while you were giving a presentation. (Meaning)
All of these elements describe the trauma vortex. In Somatic Experiencing, we find ways to allow and process that stress response by building resources for a “counter vortex.” For example, when you feel your heart begin to race, we might also be aware that simultaneously the sensation of your feet on the floor feels soft and quiet, and that when you look out the window at nature you feel a settling sensation in your abdomen. We then use these resources as we slowly work through the “trauma vortex”.
Feel safe again.
Part of Somatic Experiencing is getting more attuned to what safety feels like. For a lot of clients with developmental trauma or acute trauma, we spend a lot of time first feeling and finding safety before we start renegotiating the traumatizing experience(s).
This process can be slow as we allow the body to catch up to the mind. This avoids talking through something too quickly and coming away feeling more agitated, a desire to escape, or exhausted and drained.
As a practitioner specializing in Somatic Experiencing, my mission is to provide a safe space for you to learn to heal the intensity of your experience of past events that cause overwhelm. My aim is to help you calm and ground your nervous system in the present and implement strategies to better manage the stress that’s disrupting your health and well-being.
Who can benefit from Somatic Experiencing?
Somatic Experiencing is ideal for anyone who needs help resolving trauma related to a personal or professional experience, developmental trauma rooted in childhood, or chronic stress. Signs that you may be suffering from trauma or a stress disorder include:
- Binge eating and Disordered eating
- Food addiction
- Anxiety
- Depression
- Panic attacks
- PTSD
- Substance misuse
- Sexual dysfunction
- Sleep issues
- Anger, irritability, mood swings
- Easily startled or frightened
- An overwhelming sense of guilt, shame or self-blame
- Struggle with focus and concentration
- Feeling hopeless, sad, disconnected or numb
- Withdraw from friends and loved ones
- Gut health issues like IBD and IBS
- Aches and pains
- Muscle tension
What does a Somatic Experiencing Therapist do?
Trained to help their clients recognize how their body expresses past traumatic events through physical sensations, a somatic therapist is essentially a specialist in “body psychotherapy.”
Offering a safe space and a calm presence, a somatic therapist is instrumental in helping you grow more aware of your own bodily sensations and how your nervous system works.
A somatic therapist will also provide the tools and resources necessary to improve your coping skills and lessen the intensity and distress you feel to help achieve a stronger feeling of safety in your body.
What can you expect from a Somatic Experiencing session? Over a series of sessions, you’ll grow increasingly tolerant of the bodily sensations and emotions related to the trauma you’ve experienced.
You will not be expected to relive your trauma or discuss it in detail. Rather, your therapist will guide you between states of emotional activation and calm, helping you learn tactics to self-regulate. For example:
- Titration – helps keep physical and emotional arousal in check while processing traumatic triggers.
- Pendulation – moving between regulated parts of the body and dysregulated parts.
- Discharge – strategies to help you dissipate states of activation or arousal.
- Relaxation – techniques including breathing exercises and visualization.
Learn more. I’m a certified Somatic Experiencing Practitioner. Contact me to ask questions and learn more or you can BOOK a counseling session.




